Mole Mapping, Skin Check from 90€

Prevention of Skin Cancer

Full-body 360° examination with a personalised digital device

Detection and examination of every skin lesion and each mole separately

Detection of new and changing moles

Digital mapping for each mole with special digital microscopes

Completely painless examination & without ionising radiation
DERMADVANCE MEDICAL CLINICS
Skin moles are common, almost everyone has them. The presence of many moles, the cumulative excessive exposure to ultraviolet solar radiation, and the family history of melanoma constitute important factors to assess the risk of developing melanoma in patients with moles.
Fortunately, only a small number of moles can turn into a malignant tumour, and they rarely develop into melanoma, the most aggressive type of human cancer. Melanoma diagnosis requires experience, clinical awareness and the appropriate premium medical equipment.
The Doctor of the clinic has completed his postgraduate degree abroad focusing on early diagnosis of melanoma using the method of Dermoscopy – Mole mapping (Gratz AUSTRIA 2009).
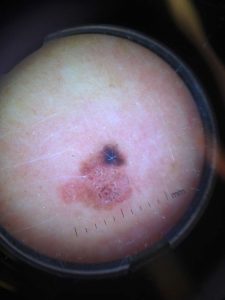
What is Dermoscopy?

Dermoscopy (dermatoscopy) is a modern non-invasive diagnostic method. In dermoscopy, special lenses and electronic devices are used, able of enlarging and emitting polarised light so as to evaluate the special morphological characteristics of the lesions under examination (colour of the lesion, pigment pattern, etc.).
This method allows the early and safe diagnosis of pigmented lesions, especially moles-nevi and melanoma.
Dermoscopy improves the rate of melanoma diagnosis by about 30%, as long as it is performed by a highly trained dermatologist with experience in this method.
Where is dermoscopy applied?
Dermoscopy was developed aiming at the early diagnosis of melanoma, the most aggressive skin cancer, which develops either on a mole (25% of the total) or on normal skin.
Improved imaging of skin structures has led to the more widespread use of dermoscopy for diagnosis and benign skin conditions, such as haemangiomas, seborrhoeic keratoses, sebaceous adenomas, etc.
What is mole mapping?
The greatest advantage of mole mapping is that it allows the detection of melanoma even at a very early stage. For the examination, which is the most effective method to detect cancer, a high-definition dermatoscope is used, as well as polarised light, which ultimately “maps” the body with perfect accuracy, focusing on the moles.
Using this complete method, these images of the moles, your doctor can make an accurate diagnosis and future comparisons, always based on digital means.
There are many specific dermatoscopic characteristics for melanoma and other skin cancers that can be detected with dermoscopy, but are not visible to the naked eye.
Moreover, with the recall option, images can be re-examined and digital comparisons with new images from follow-up examinations are possible. In addition, image processing and evaluation using a special software that assesses – classifies the lesion as high or low risk plays a crucial role in the whole process.
When should I have mole mapping?
If you belong in one of the following groups, mole mapping may be essential
- Persons with multiple – dysplastic moles
- Persons with a family or personal history of melanoma
- Immunocompromised patients
What equipment is used for mole mapping at the medical office?
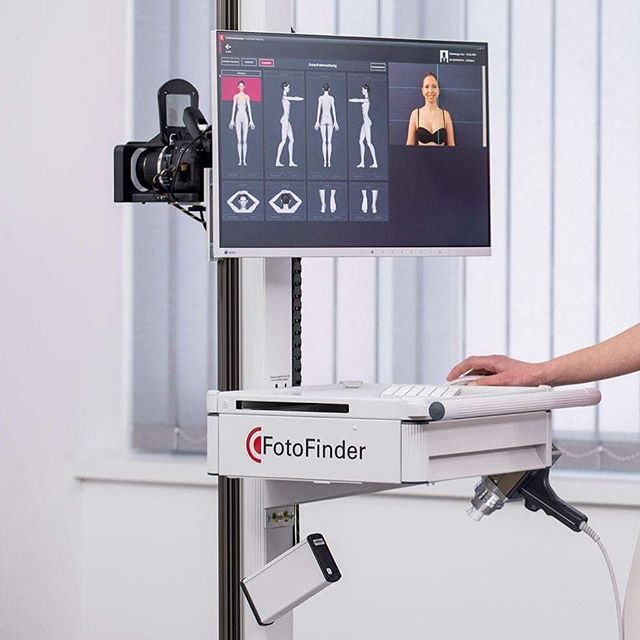
At the medical office, we use the latest, high-tech Fotofinder Vexia system, with the following characteristics:
Fotofinder Moleanalyzer. In mole mapping, sensitivity and specificity are critical for the reliability of a result. If sensitivity is greater than 90%, usually specificity is affected, leading to increased excision of benign moles.
Fotofinder Moleanalyzer has been developed in collaboration with the Dermatology Department of the University of Tübingen and provides both high sensitivity and specificity.
It is not intended to replace the doctors, just to offer a second, computer-assisted opinion, based on clinically tested pattern recognition algorithms with risk rating. This offers – especially in abnormal cases – even greater safety in the timely diagnosis of malignant melanoma.
- Analysis of melanocytic nevi using pattern recognition algorithms
- Reliably high level of sensitivity and specificity
- Incredible imaging of structural changes
- Parallel analysis of two lesions to quantitatively determine the changes
Fotofinder Bodyscan. Skin analysis using the Bodyscan software is a basic component of the overall body mapping procedure. The advanced system compares automatically the current full-body photographs with the ones from the previous examination, and marks the changes at a glance. This allows Bodyscan to assist you in the detection of melanoma as early as possible and be confident that nothing will go unnoticed. With the new Bodyscan ATBM, Fotofinder has improved the automatic comparison of primary nevi and image monitoring again.

The results are now ready as soon as the capturing is finished and can be shown or hidden at any time. The new procedure does not involve any distortion of the original images and accelerates the mole mapping procedure considerably!
- Reliable system for identifying changes in the skin
- Automatic comparison of two overview images from the total mole mapping procedure
- Coloured marking of new and changed lesions
What are the benefits of mole mapping?
Regular and accurate monitoring with mole mapping is the best way to prevent melanoma.
Early detection of any dangerous and new nevi. Digital imaging and the special software allow the detection of even the slightest difference is the structure of moles.
Consecutive annual tests are perfectly painless – without irradiation – and help us in avoiding unnecessary mole removals.
Nevi (Moles) Evaluation
Moles, brown spots and growths on the skin are usually harmless, but not always. Anyone who has more than 100 moles is at greater risk for melanoma. The first signs can appear in one or more atypical moles. That’s why it is so important to get to know your skin very well and to recognise any changes in the moles on your body. Below, the ABCDE method for the evaluation of moles is presented. If you see one or more signs, you should make an appointment with a dermatologist immediately.
Α – Asymmetry A benign mole is not asymmetrical. If you draw a line through the mole and the two halves do not match, it indicates that it is asymmetrical. Asymmetry is a warning sign for melanoma.
Β – Border A benign mole has smooth, even borders, unlike melanomas. The borders of an early melanoma tend to be uneven. The edges may be notched.
C – Colour Most benign moles are all one colour – often a single shade of brown. Colour changes or the presence of a variety of colours is another warning signal. A melanoma may also become red, white or blue .
D – Diameter Benign moles usually have a smaller diameter than malignant ones. Melanomas usually are around 6 mm, but they may sometimes be smaller when detected early.
Ε- Evolving Benign moleslook the sameover time. When a mole isevolving, see a doctor. Any change in size, shape, colour, elevation, or another trait, or any new symptom such as bleeding, itching or dryness are considered dangerous indications.
Other warning signs:
• Appearance of a new mole • Colour extending in the surrounding skin • Redness or swelling beyond the nevus • Pain • Sensitivity • Itching • Bleeding • Scaly appearance
What are the risk factors for skin – cancer – melanoma?
High-Risk Individuals
A risk factor is anything that affects your chance of getting a disease such as cancer. Different cancers have different risk factors. Some risk factors, like smoking and excessive sun exposure, can be changed. Others, like a person’s age or family history, cannot be changed. But, having a risk factor, or even several risk factors, does not mean that one will get the disease. Some people who get the disease may have no known risk factors. Some of the risk factors are discussed below; people with the following or who are exposed to these are classified as high-risk and should have their moles tested regularly.
Prolonged sun exposure / sunburns during childhood. (Exposure to ultraviolet (UV) rays is a major risk factor for most melanomas. Sunlight, tanning beds and sun lamps are sources of UV rays. UV rays damage the DNA of skin cells, and skin cancer begins when this damage affects the DNA of genes that control skin cell growth.
Moles – Nevi A mole is a benign, non-cancerous pigmented tumour. Babies are not usually born with moles; they often begin to appear in children and adolescents. Most moles will never cause any problems, but someone who has many moles is more likely to develop melanoma.
Dysplastic nevi (Atypical moles) (These moles look a little like normal moles but also have some features of melanoma. They are often larger and have an abnormal shape or colour)
Dysplastic nevus syndrome: People with this inherited condition have many dysplastic nevi and at least one close relative who has had melanoma. People with this condition have a very high lifetime risk of melanoma, so they need to have very thorough, regular skin exams.
Fair skin, freckling, and light hair: The risk of melanoma is much higher for people with fair skin, red or blond hair, blue or green eyes, or fair skin with freckles or skin that burns easily.
Family history of melanoma. (The risk of melanoma is higher if one or more first-degree relatives has had melanoma. Around 10% of all people with melanoma have a family history of the disease.)
Weakened immune system. (People with weakened immune systems (from certain diseases or medical treatments) are more likely to develop many types of skin cancer, including melanoma.)
Age. Melanoma is more likely to occur in older people.

