What is Vitiligo?
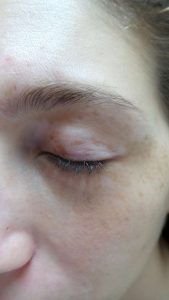 Vitiligo is a disease in which the pigment cells of the skin, melanocytes, are destroyed in certain areas of the body.
Vitiligo is a disease in which the pigment cells of the skin, melanocytes, are destroyed in certain areas of the body.
Vitiligo leads to depigmented, or white, patches of skin in any location on the body. Vitiligo can be focal and localised to one area, or it may affect several different areas on the body.
The exact cause of vitiligo is unknown, although most experts believe that it is an autoimmune condition in which the body’s immune system mistakenly attacks and destroys certain cells within the body.
This happens because the body’s melanocytes are destroyed. Vitiligo may also affect the mucous membranes (such as tissue inside the mouth and nose) and the eyes.
Your Dermatologist can diagnose this “loss of pigment”, while pigment loss may appear anywhere on our body, such as:
- skin
- hair (scalp, eyebrows, eyelashes, beard)
- inside the mouth
- genitals
Most people who suffer from vitiligo lose the colour of their skin. The affected skin may become lighter or completely white. Many patients have no other symptoms and feel healthy. Certain patients report that the affected skin with vitiligo is itching or painful.
What causes vitiligo?
The exact cause of vitiligo is unknown, although most specialists consider it an autoimmune disease. An autoimmune disorder occurs when the body’s immune system attacks and destroys healthy body tissue.
In the case of vitiligo, the immune system attacks the melanocytes of the skin. It is also possible that one or more genes make a person more prone to the manifestation of this skin conditions.
Some researchers think that the melanocytes destroy themselves. Others think that a single event such assunburnor emotional distress can cause vitiligo. But these events have not been proven to cause vitiligo.
- Most people who have vitiligo will develop the condition prior to age 40 & about half develop it before age 20.
- Vitiligo tends to run in families.
- Vitiligo is sometimes associated with other medical conditions, including thyroid dysfunction.
- Vitiligo is not painful and does not have significant health consequences; however, it can have emotional and psychological consequences.
- Some medical treatments can reduce the severity of the condition, but it can be difficult to cure.
Symptoms of Vitiligo
The main sign of vitiligo is the loss of colour, producing light-coloured or white patches on the skin. Usually, depigmentation is initially observed in areas where the skin is exposed to the sun, such as the hands,feet, arms, face, and lips.
Signs of vitiligo:
- Skin depigmentation
- Premature whitening or greying of the hair on your scalp, eyelashes, eyebrows or beard (usually before the age of 35)
- Loss of colour in the tissues that line the inside of your mouth and nose (mucous membranes)
- Loss of or change in colour of the inner layer of the eyeball (retina)
- Discoloured patches around the navel, armpits, rectum, and genitals
Vitiligo has different types and categories. Today, most doctors recognise the following types:
- Generalised Vitiligo
- Segmental Vitiligo
- Localised or Focal Vitiligo
Depending on the type of vitiligo, Depigmentation(s) may affect:
- Many parts of the body. With this most common type, called generalised vitiligo, the discoloured patches often progress symmetrically on corresponding body parts.
- Only one part or side of the body. This type, called segmental vitiligo, tends to occur at a younger age, progress for a year or two, and then stop.
- One or a few areas of the body. This type is called localised or focal vitiligo.
It is difficult to predict how the disease will progress. Sometimes the patches stop forming without treatment. In most cases, pigment loss spreads progressively (slowly or faster), affecting the greatest part of your skin. Rarely, the skin gets its colour back.
How do dermatologists diagnose vitiligo?
If your dermatologist thinks that you may have vitiligo s/he will:
- Check your medical history, and make specific questions, such as whether someone in your family has vitiligo.
- Examine carefully the affected skin.
- Examine the affected skin with Wood’s lamp, a special lamb emitting light at specific wavelength, making the lesions of vitiligo visible, even the lighter and just appearing lesions.
- Blood tests may be also required to check your thyroid gland function. People who have vitiligo often suffer from a thyroid autoimmune disease. A blood test will demonstrate whether your thyroid is healthy.
Who is affected by vitiligo?
Millions of people around the world have vitiligo. About half of vitiligo patients are diagnosed before the age of 20, and most patients who get the disease will have it for the rest of their lives. Only rarely vitiligo goes away on its own.
Vitiligo occurs in individuals of all skin colours and races. It affects men and women fairly equally.
The risk of vitiligo is increased in persons with:
- A close relative with vitiligo.
- An autoimmune disease, especially Hashimoto’s disease (a thyroid disease) oralopecia areata (causes sudden hair loss).
Treatment of Vitiligo – 7 Treatment Approaches
Many treatments are available to help restore skin colour or even skin tone. Results vary and are unpredictable. Some treatments have serious side effects. Therefore, your doctor may suggest that you first try improving the appearance of your skin by applying self-tanning products or makeup.
If you decide to treat the condition with a drug or other therapy, the process may take many months to judge its effectiveness. And you may have to try more than one approach or a combination of approaches before finding the treatment that works best for you.
The type of vitiligo treatment that is best for your will depend on your preferences, your general health, age and the areas where vitiligo is present on your body.
Α. Non-medical management of Vitiligo
- Cosmetic options include makeup and the use of self-tanner (sunless tanning product).
- Offer a safe option to make vitiligo less visible.
- Often recommended in children, because possible drug side effects are avoided.
- Disadvantages: Repeated application is required, time-consuming process, and the result is rarely absolutely natural.
Β. Topical Therapy
- Many different substances can give skin its colour back.
- Indicated for small areas.
- The most commonly prescribed drugs are potent or very potent topical corticosteroids. Skin colour is restored in approximately 45 percent of patients after 4 to 6 months of treatment.
- A topical corticosteroid may be combined with another medicine to improve the results.
- Topical therapy for vitiligo works better in persons with dark skin tones.
- Topical preparations are more effective in certain parts of the body, such as the face. They are less effective when applied on the hands and feet.
- Not all topical preparations are appropriate for use on the face.
- Disadvantages: These drugs have possible side effects, and therefore patients should be closely monitored. A possible serious side effect of topical corticosteroids for a long period of time (a year or more) is skin atrophy. This means that the skin becomes thin and fragile, while spider veins may also appear.
Γ. Phototherapy – Light Therapy
- Use of light at specific wavelength to re-pigment the skin.
- Treatment in phototherapy cabin or with the ECXIMER Laser, depending on the area with vitiligo.
- Phototherapy works better on the face, but it is less effective on the hands and feet.
- It is considered an effective treatment for a large proportion of patients; approximately 70 % have good results with the use of Excimer Laser.
- The results may not be permanent. Approximately half, 44 percent of patients, relapse within 1 year of treatment discontinuation. After 4 years, about 86 percent has lost a little colour compared to that restored with phototherapy.
- Time commitment is required. Patients need 2 or 3 treatments per week for several weeks.
- It can be combined with another treatment, such as topical corticosteroids.
Δ. Chemophototherapy (PUVA)
- Uses UVA spectrum light and a suitable photosensitising agent called psoralen to restore skin colour.
- Psoralen may be applied to the skin (topical PUVA or bath PUVA) or taken as a pill.
- It is a treatment option for generalised vitiligo.
- It is 50% to 75% effective in restoring vitiligo on the face, trunk, arms, and the proximal portion of the lower limbs.
- It is not very effective regimen for hands (palms and fingers) and feet (soles and toes).
- Treatments are time-consuming because transfer to a hospital of PUVA centre is required twice a week for about 6 months.
- Psoralen may affect the eyes and therefore treatment eye examination is required both before and after the treatment.
- To avoid serious side effects, patients should be closely monitored by a dermatologist.
Ε. Surgery
- This is the last therapeutic option when all other methods have failed.
- It is recommended in adults with vitiligo that is stable for at least 6 months.
- It is not indicated in children.
- It is not indicated in persons prone to develop keloids or hypertrophic scars.
- Various surgical interventions are available. In most, skin grafting is employed in skin areas or hair follicles and areas with normal pigmentation are transferred to areas with vitiligo.
- It is effective for 90 to 95% of the patients.
- Topical infection, repigmentation failure and the appearance of poikiloderma are common possible side effects.
ΣΤ. Alternative therapies
- Certain vitamins, minerals, amino acids and enzymes have been considered helpful in treating vitiligo.
- There is not enough evidence to support these vitiligo treatments and no knowledge of possible side effects.
- The herb Ginkgo biloba has been studied in clinical trials. The results from a study demonstrated that the herb can restore vitiligo skin colour to and stop worsening.
- If you follow a treatment to restore lost skin colour, it is possible that the colour will be restored slowly or not completely. Sometimes, this treatment is not effective.
Ζ. Depigmentation
- This treatment removes the remaining pigment from the skin.
- Very few patients are eligible for this treatment.
- Destroying the remaining pigment leaves the skin perfectly white.
- It may be an option for an adult who only has very few areas of the body with pigment, and no other treatment for vitiligo has been effective.
- To remove the remaining colour, the use of a cream is required, applied once or twice daily. This cream removes progressively the pigment from the skin.
- Treatment through Depigmentation may last from 1 to 4 years.
Treatment Results
It is not possible to predict how a patient will respond to vitiligo treatment. It is important to keep in mind that no one treatment works for everyone. Results can vary from one part of the body to another. When combining two or more treatments delivers a better result.
Frequently Asked Questions… and Answers
Can a child with vitiligo be treated?
Yes, but some treatments are not suitable for children. The following are options for a child:
- Topical corticosteroids
- For children with generalised vitiligo, narrow-band UVB phototherapy is a good option
- PUVA is not indicated in children below the age of 12. Even then, the risk and benefits of this treatment should be carefully considered.
Do scientists perform research for a more effective treatment for vitiligo?
Yes, through the study of the genes involved in vitiligo. Scientists believe that if the involved genes are identified, they will find what destroys the cells that give skin its colour. Knowing this, it will be possible to develop more effective treatments for vitiligo. One of the main goals of this research is to develop a treatment that will permanently stop skin pigment loss.
Tips for Patients with Vitiligo
Dermatologists share the following tips with their patients with vitiligo.
Protect your skin from sun. Each individual with vitiligo can benefit from sun protection because:
- Skin that has lost its colour sunburns very easily.
- A bad sunburn can worsen vitiligo.
- If your skin is fair, avoiding suntan makes vitiligo less visible.
To protect your skin from the sun:
- Apply a generous amount of sunscreen every day on your skin, on areas that will not be covered by your clothes. Use a sunscreen that offers:
- UVA / UVB protection (the label may indicate “broad-range”)
- Sun Protection Factor (SPF) 30 or more
- Water-resistant
- Apply sunscreen every day at least 15 minutes before going outdoors.
- Reapply sunscreen when outdoor, every 2hours, even on cloudy day.
- Wear clothing that protects your skin from the sun (with dense weave, like a pair of jeans). A long-sleeve denim shirt has an SPF of about 1 700. A white t-shirt only has an SPF 7, and a green t-shirt has an SPF 10.
- Seek Shade, especially during the noon, when the sun’s damaging rays are at their strongest and you are likely to sunburn.
- Do not use tanning beds and sun lamps.
- Don’t get a tatoo. Getting a tattoo can cause something called the Koebner phenomenon or Keobnerisation. This is actually reappearance of vitiligo at this area, which may occur about 10 to 14 days later.
The emotional aspects of having vitiligo are often overlooked, but they are a real and serious problem. If a child has vitiligo children may tease and bully. People may stare at you or avoid you. Studies conclude that many people who have vitiligo have a decreased quality of life.
Being in contact with other people with vitiligo can help. You may find support group links online.


